 The largest clinical trial of its kind – the EVOLVE kyphoplasty study – tracked the results of 350 back pain patients who underwent balloon kyphoplasty.
The largest clinical trial of its kind – the EVOLVE kyphoplasty study – tracked the results of 350 back pain patients who underwent balloon kyphoplasty.
The study began with baseline measurements before kyphoplasty was completed.
Then starting at 7 days after surgery and for the next 12 months »
Patient outcomes were studied at intervals to better understand short-term and long-term effectiveness of the kyphoplasty procedure.
The study definitively answers questions such as:
- Does kyphoplasty work?
- What is the success rate of kyphoplasty?
- What is the pain rate after kyphoplasty?
- How does kyphoplasty affect mobility?
- What are the expected outcomes of kyphoplasty?
Let’s take a look…
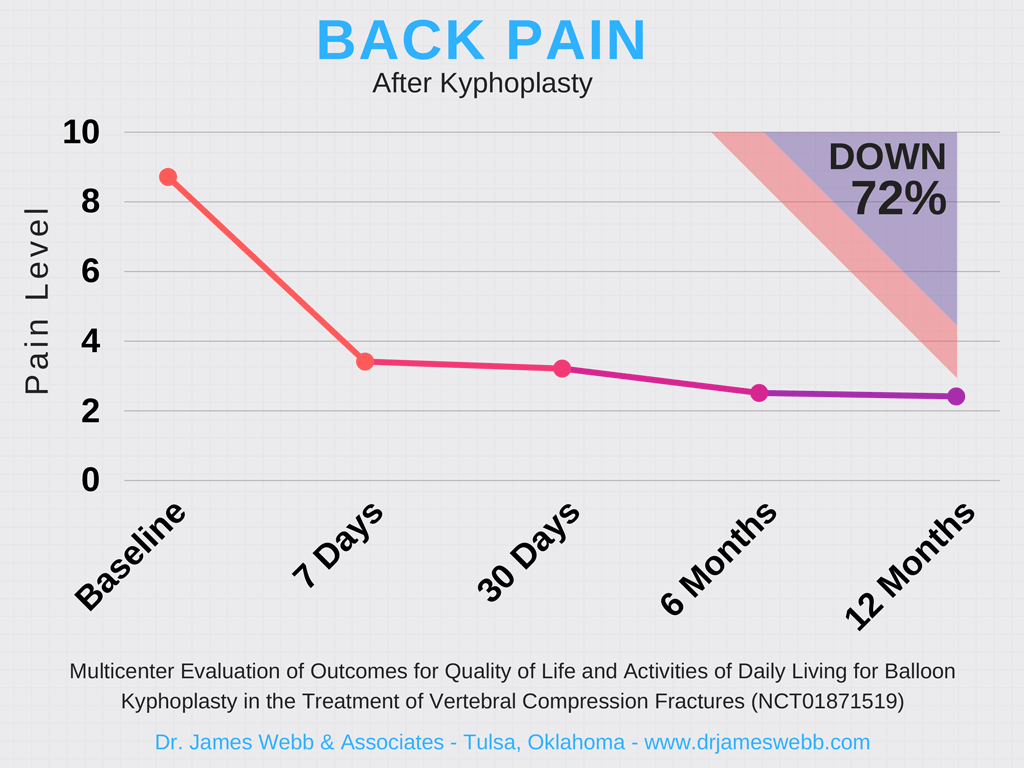
Successful patient outcomes following kyphoplasty include:
- 72% Improvement in back pain
- 59% Improvement in back function
- 58% Improvement in quality of life
- Increased mobility (including the ability to walk without aid)
- Increased ability to self-manage activities of daily living
- Reduced opioid use for pain management
Study results confirm the effectiveness of kyphoplasty as a powerful treatment option for severe back pain and loss of back function in osteoporosis patients.
In this article, we will dive deep into other findings of the EVOLVE kyphoplasty study to better understand the outcomes patients experienced following kyphoplasty.
Dr. James Webb & Associates role in the study
 Dr. James Webb M.D. – a musculoskeletal radiologist who specializes in osteoporosis treatment and interventional pain management in Tulsa, Oklahoma – was a principal investigator in the EVOLVE study, with 40 study participants receiving kyphoplasty treatment at Dr. Webb’s office in Tulsa.
Dr. James Webb M.D. – a musculoskeletal radiologist who specializes in osteoporosis treatment and interventional pain management in Tulsa, Oklahoma – was a principal investigator in the EVOLVE study, with 40 study participants receiving kyphoplasty treatment at Dr. Webb’s office in Tulsa.
“When the data came rolling in, even we (the physicians) were astounded by the results. We knew by observation that our patients get better with kyphoplasty. We knew their pain got better, that mobility improved, their functional status improved, their posture improved, everything. But seeing statistical improvement demonstrated on every single endpoint in a controlled clinical trial is another thing altogether,” noted Dr. Webb.
What are Spinal Fractures?
Spinal fractures (or vertebral compression fractures) are caused by loss of bone density.
Bone density loss is attributed to osteoporosis, the most widespread degenerative disease in the developed world.
Although studies show approximately 1 in 2 women and 1 in 5 men over 50 will break a bone due to osteoporosis, it remains one of the most under-diagnosed conditions in the world.
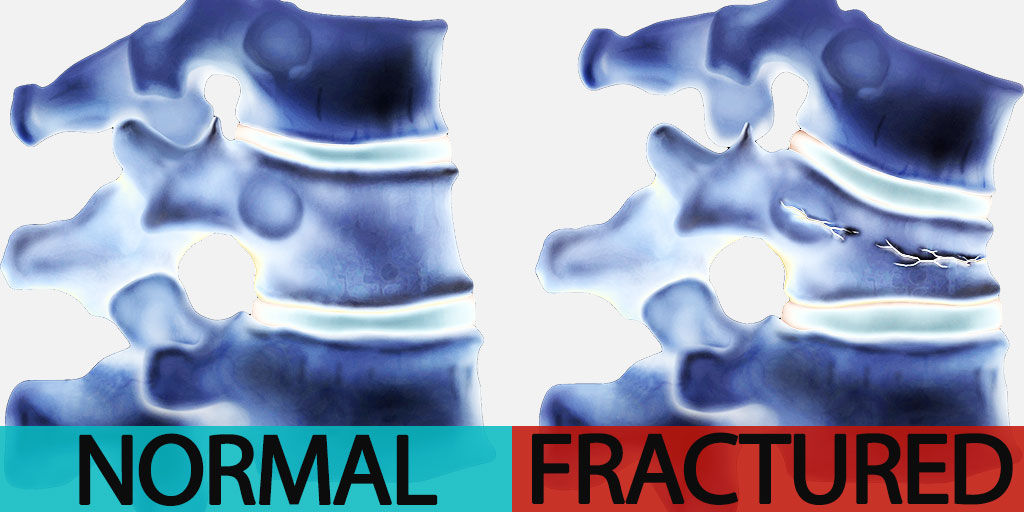
Osteoporosis has been called a “silent disease,” because many people don’t know they have osteoporosis till their first fracture.
And even after a vertebral compression fracture occurs, it often goes untreated. Spinal fractures may happen as a result of trauma or may take time to develop, resulting in a condition called “Kyphosis” recognizable by a rounded back.
Sometimes called the “dowager’s hump,” this condition compresses the abdomen and chest and causes severe pain in the back, sides, and rib areas.
Left untreated, osteoporosis can lead to depression, loss of mobility, and loss of the ability to care for oneself.
Many patients eventually require long-term nursing home care.
What is Kyphoplasty?
Balloon kyphoplasty is a minimally invasive outpatient procedure used to treat painful, acute vertebral compression fractures (VCF) associated with osteoporosis or cancer.
During the procedure collapsed vertebrae are filled with a special bone cement to restore the shape and strength of the vertebral body.
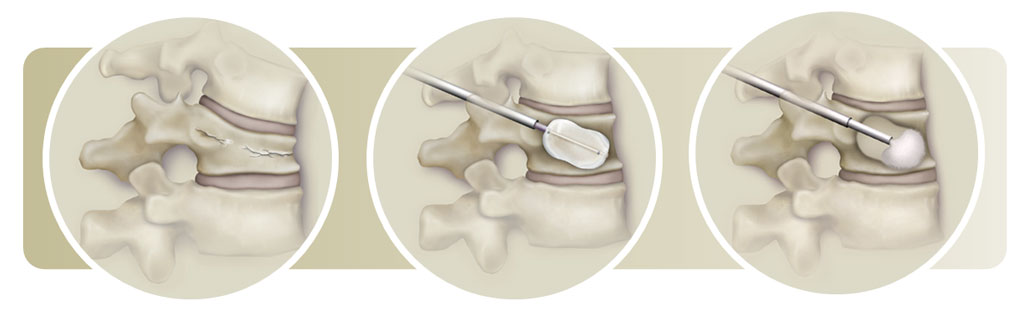
Photo Credit: Medtronic
During balloon kyphoplasty, a needle is inserted into the compressed vertebrae.
A balloon is inserted through the needle into the vertebral body then inflated to create a cavity and gently lift the bone sections into the normal position.
The cavity created from the balloon is then filled with orthopedic cement – a bone cement technically know as polymethylmethacrylate (PMMA) – which hardens quickly to create an internal cast, stabilizing the bone.
Numerous studies have been done on kyphoplasty. It is one of the best studied procedures in scientific literature related to the spine.
With over 19,000 scientific articles on kyphoplasty, the evidence has been overwhelmingly positive.
Kyphoplasty has been shown as a superior osteoporosis treatment for pain control, while reducing the risk of other fractures, restoring function, and actually saving lives.
Kyphoplasty vs. Vertebroplasty
Kyphoplasty and vertebroplasty are both medical procedures designed to treat pain associated with vertebral compression fractures. Where Kyphoplasty first uses a balloon to restore vertebral height, vertebroplasty does not. Kyphoplasty has a significantly lower complication rate compared to vertebroplasty and has an added life-extending benefit as it decreases mortality.
About the EVOLVE Kyphoplasty Study
The EVOLVE study (NCT01871519) followed 350 participants who underwent balloon kyphoplasty at one of 25 spine treatment facilities throughout the United States.
Spine Treatment Study Locations
Alabama Clinical Therapeutics, LLC
University of Alabama at Birmingham
Washington Radiologist Medical Group
Sutter Health Sacramento Sierra Region
Alta Orthopaedic Medical Group
Torrance Memorial Medical Center
Radiology Imaging Specialist of Lakeland
The Back Center
Physicians & Surgeons of Pocatello
St. Luke's Health System
Central Illinois Neuroscience Foundation
Adventist Health Partners
Presence Saint Joseph Medical Center
Illinois Bone & Join
Indiana Spine Group
Advanced Diagnostic Imaging, PC
Beaumont Health System
Premier Radiology
Sierra Regional Spine Institute
Consulting Orthopaedic Associates, Inc
Clinical Investigations, LLC
Dr. James Webb & Associates
NeuroSpine Institute, LLC
Scoliosis & Spine Surgery Clinic of Memphis, PLLC
The West Clinic
The objective of the study was to collect and report on outcomes pertaining to activities of daily living, quality of life, and safety parameters in a Medicare population to be treated with balloon kyphoplasty in the treatment of painful, acute, vertebral body compression fractures (VCFs) associated with either osteoporosis or cancer.
Principal investigators included some of the nation’s most experienced physicians in the fields of bone health and kyphoplasty treatment.
The study examined four primary outcomes:
- Back Pain – measured using the NRS scale where patients rate the severity of back pain on a scale of 0 to 10, where 0 represents “no pain” and 10 represents “pain as bad as it could be”
- Back Function – measured using an ODI questionnaire to assess patient back function on a scale of 0 to 100, where 0 represents “no disability” and 100 represents “maximum disability”
- Quality of Life – measured using the 36-question Short Form Health Survey to assess quality of life on a scale from 0 to 100, with higher scores denoting better quality of life
- General Health Status – measured by the EQ-5D index, to assess overall health and well-being through a questionnaire and medical evaluation on a scale of 0 to 1.0, where 0 = death and 1.0 = perfect health
Study participants were evaluated using the above measures prior to surgery and at intervals following surgery at – 7 days, 30 days, 3 months, 6 months, 9 months, and 12 months.
Participants included Medicare patients with an average age of 78.9 years old.
Of the participants 77% were women, and 23% were men.
All participants had one or more vertebral compression fractures caused by osteoporosis or cancer, with the majority (343 of 350) of VCF caused by osteoporosis.
EVOLVE Study Results
“We found statistically significant improvement in every single measured outcome at every single follow up point. Every single data point didn’t just show improvement, but statistically significant improvement which is a scientific measure of certainty.” -Dr. James Webb, M.D.
All improvements were statistically significant with a P-value less than .001.
The findings of this study demonstrate that kyphoplasty results in across the board improvements in back pain, back function, quality of life, and general health.
Sustained Back Pain Relief
The fact that patient back pain relief was statistically significant even after a year is amazing, because once a patient suffers vertebral fractures, their risk for getting additional fractures increases exponentially.
In addition to showing long-term, sustained back pain relief with kyphoplasty – study results also showed patients reported immediate back pain relief and improved back function.
In fact, measured at just 7 days after kyphoplasty treatment, patients rated back pain had dropped to just 3.4 (on a scale of 0 to 10) versus 8.7 before treatment.
And back pain continued to drop throughout the duration of the study.
Back Pain Before & After Kyphoplasty
| Timeline | Participants Analyzed | Pain Rating |
| Back pain at baseline | 350 | 8.7 |
| Back pain at 7 days | 340 | 3.4 |
| Back pain at 30 days | 315 | 3.2 |
| Back pain at 6 months | 265 | 2.5 |
| Back pain at 9 months | 277 | 2.3 |
| Back pain at 12 months | 257 | 2.4 |
Improved Back Function
In addition to significant reduction in back pain, the study also observed demonstrated improvement in back function, measured by the Owestry Disability Index (ODI).
The ODI score is determined through the use of a questionnaire presented by clinicians to quantify the level of disability associated with back pain.
The self-completed questionnaire contains questions related to the following topics: intensity of pain, ability to walk, ability to sit, sexual function, ability to stand, social life, sleep quality, and ability to travel.
The results of the questionnaire are summarized into an ODI score ranging from 0 to 100.
ODI Scoring Ranges
- 0 – 20: Minimal disability
- 21 – 40: Moderate disability
- 41 – 60: Severe disability
- 61 – 80: Crippling disability
- 81 – 100: Bed bound or exaggeration of symptoms
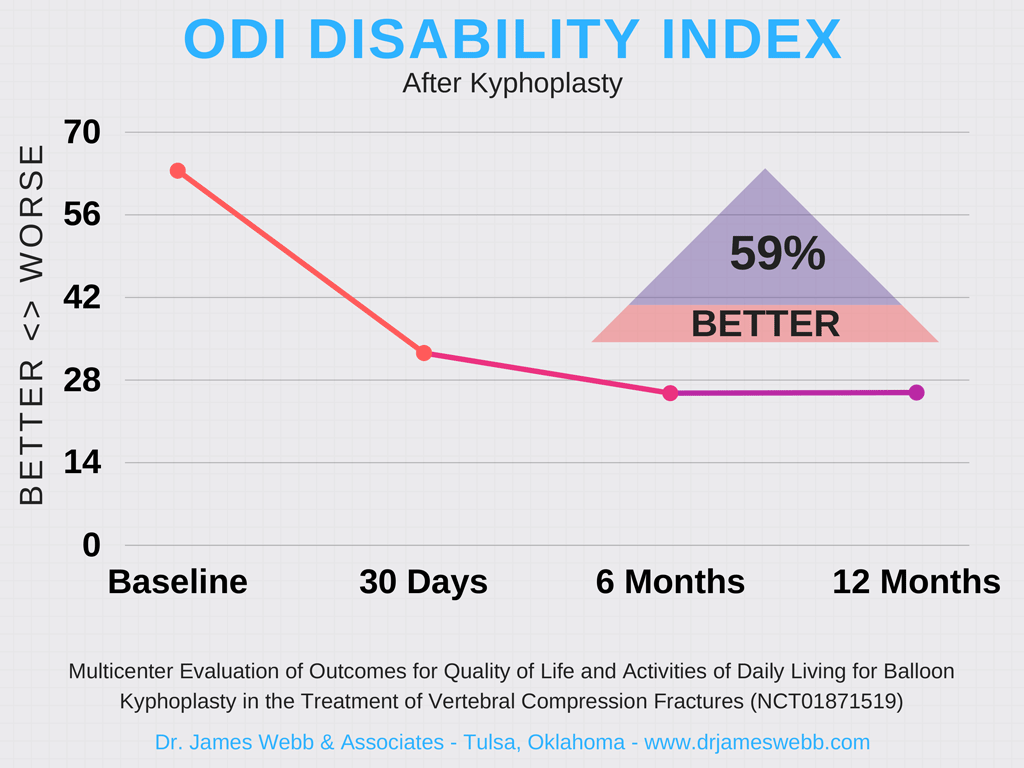
Prior to Kyphoplasty the average ODI score for study participants was 63.4, putting them in the crippling disability range.
Just 30 days after Kyphoplasty, the average ODI score for study participants had dropped sharply to 32.5, designated as a moderate disability.
In subsequent follow-ups, back function continued to improve, with ODI scores at 25.8 after 12 months.
Back Function Before & After Kyphoplasty
| Timeline | Participants Analyzed | ODI Score |
| Back function at baseline | 350 | 63.4 |
| Back function at 30 days | 304 | 32.5 |
| Back function at 6 months | 255 | 25.7 |
| Back function at 12 months | 247 | 25.8 |
Improved Quality of Life
The study measured quality of life using the Short Form Health Survey.
The 36-question SF-36v2 health survey measures functional health and well-being. The survey includes questions, such as:
- In general, how would you say your health is?
- Does your health now limit you… in climbing stairs? Bathing and dressing yourself? Bending, kneeling, or stooping?
- How much of the time during the past 4 weeks… did you feel full of life? Did you have lots of energy?
The answers to these questions create a score on a scale from 0 to 100, with higher scores denoting better quality of life.
Quality of Life Before & After Kyphoplasty
| Timeline | Participants Analyzed | SF-36v2 Score |
| Baseline | 350 | 24.2 |
| 30 days | 304 | 34.9 |
| 6 months | 255 | 37.6 |
| 12 months | 246 | 38.2 |
Quality of life made an immediate jump 30 days after kyphoplasty, and patients reported continued improvement throughout the duration of the study.
Ability to Manage Daily Living
In addition examining overall quality of life, the study looked at specific areas, such as daily living activities and bed rest.
Here’s a look at how kyphoplasty removed limitations on daily living activities.
You’ll note that before the kyphoplasty procedure, 96.3% of participants reported limitations to daily living activities due to back pain in the previous two weeks.
After 3 months, just 28.9% reported limitations.
Daily Living Activities Limited Due to Back Pain
| Timeline | Participants Analyzed | Percent |
| Baseline | 350 | 96.3 |
| 30 days | 304 | 53.3 |
| 3 months | 283 | 31.8 |
| 6 months | 255 | 31.0 |
| 12 months | 246 | 28.9 |
Also noteworthy is the fact that kyphoplasty helped patients avoid immobilization due to bed rest.
That is a great thing, because bed rest affects every system in the human body and can lead to other debilitating (and life-threatening) conditions.
Kyphoplasty resulted in an 88% reduction in bed rest due to back pain.
Days of Bed Rest Due to Back Pain
| Timeline | Participants Analyzed | Days of Bed Rest |
| Baseline | 350 | 6.0 |
| 30 days | 304 | 1.5 |
| 3 months | 283 | 0.7 |
| 6 months | 255 | 0.7 |
| 12 months | 246 | 0.7 |
Improved Overall Health Status
The EVOLVE kyphoplasty study showed incredible improvements in multiple areas of patient health.
Changes in overall health status were tracked using the EQ-5D Index Score, a measure of general health status and well-being.
The EQ-5D Index Score looks at 5 “dimensions” of health: mobility, self-care, usual activities, pain/discomfort, and anxiety/depression.
The index score is calculated through a questionnaire and medical evaluation and is based on a scale of 0 to 1.0, where 0 = death and 1.0 = perfect health.
Overall Health Before & After Kyphoplasty
| Timeline | Participants Analyzed | EQ-5D Score |
| Health status at baseline | 350 | 0.383 |
| Health status at 30 days | 304 | 0.710 |
| Health status at 6 months | 255 | 0.756 |
| Health status at 12 months | 247 | 0.758 |
The data shows that not only does Kyphoplasty result in direct benefits associated with back pain relief and back function, but it also improves the patient’s overall health and well-being.
Conclusion
“What the EVOLVE trial does is unequivocally show that in the most experienced hands, kyphoplasty is a safe, effective and long-lasting procedure for treating patients with painful vertebral fractures from osteoporosis in the Medicare population,” Dr. Webb said.
If you or a loved one is suffering from osteoporosis, kyphosis, a spinal fracture, or unexplained back pain (even if you’ve already had back surgery) »»
Contact our office to request an appointment
Dr. Webb & Associates is a spine treatment facility located in Tulsa, Oklahoma, helping patients optimize bone health and treat the underlying causes of back pain without invasive surgery or pain medications.
Content Attribution: You are welcome to share graphics, charts & partial quotes. Please provide attribution with a link back to this article. Do not copy full text contents.

